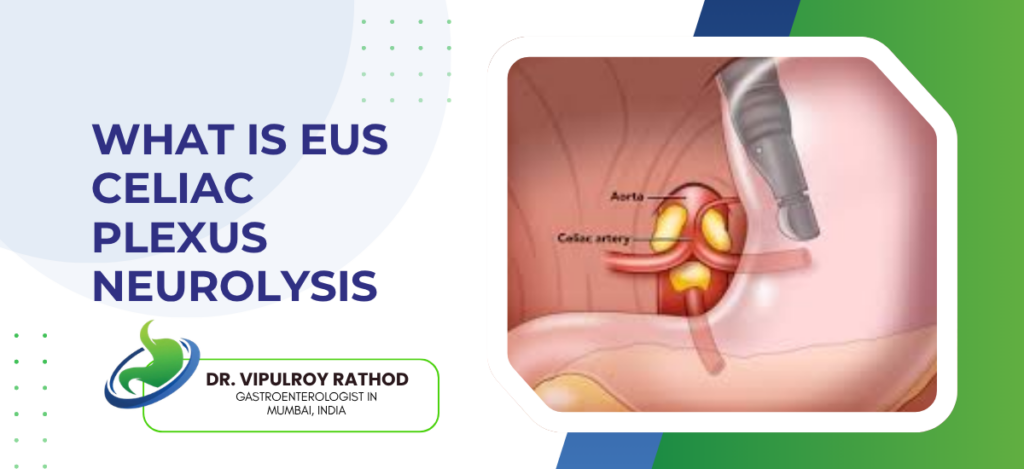
EUS celiac plexus neurolysis (CPN) is a minimally invasive procedure where alcohol is injected into the celiac plexus nerve cluster under endoscopic ultrasound guidance to permanently block pain signals from the pancreas, used primarily for pancreatic cancer pain that medication isn’t controlling, it works because it disrupts the nerve pathway at source rather than trying to suppress signals that keep firing regardless of what’s prescribed.
According to Dr. Vipulroy Rathod, an experienced Gastroenterologist in Mumbai,
“Celiac plexus neurolysis through EUS is one of the most impactful interventions available for pancreatic cancer pain because it targets the nerve pathway itself rather than just masking the pain with medication that stops working as disease progresses.”
What Do Patients Actually Experience Before and After?
Understanding the procedure honestly changes the decision-making for patients and families in ways that vague reassurance never does.
- Procedure: Sedation, scope into stomach, EUS finds the celiac plexus in real time, injection takes a few minutes once position is confirmed, total time 30 to 45 minutes, home same day and most people are surprised by how straightforward it actually was compared to what they imagined.
- Relief: Pain reduction within 24 to 72 hours in most cases, not all patients get complete relief but most get significant improvement, and the reduction in opioid dose that follows often resolves the nausea and constipation that heavy pain medication was causing on top of everything else.
- Risks: Temporary pain flare or diarrhoea in first 48 hours, hypotension occasionally, serious complications like paralysis are rare but real and this procedure should only be done by someone who’s performed enough of them to handle whatever comes up without sending the patient to a different team.
- Repeat: One session handles most patients for months, pain eventually returns as disease progresses, repeat neurolysis or transition to other palliative strategies decided based on how long the first response held and where the overall clinical picture sits at that point.
This procedure doesn’t treat the cancer but it gives patients their life back during a period when that matters more than most people outside the situation understand. Read more on pancreatitis to see how EUS-guided intervention handles pancreatic conditions beyond just cancer pain relief.
Why Does MASLD Diagnosis Actually Matter?
Finding fat on a liver scan is where the investigation starts, not where it ends, and most patients have no idea what comes next.
- Stage: Simple steatosis carries low progression risk while MASH carries real fibrosis risk, and without staging through fibroscan, blood markers, or biopsy the patient has no idea which end of the spectrum they’re on or how urgently they need to act on it.
- Metabolic: MASLD means the underlying drivers, obesity, diabetes, insulin resistance, dyslipidaemia, need active management not just a lifestyle leaflet handed over at the end of a consultation nobody follows up on because nobody made it a clinical priority.
- Progression: Around 20% of MASLD patients with steatohepatitis progress to significant fibrosis over time and a proportion reach cirrhosis and liver cancer risk, so the patient told they have fatty liver and sent home without staging is in a completely different position from the patient properly managed from the start.
- Cardiovascular: MASLD carries significant cardiovascular risk independent of liver disease because the metabolic syndrome driving liver fat accumulation is the same syndrome driving heart disease, and patients with MASLD die of cardiovascular events more often than liver complications in early stage disease.
Fatty liver report without staging and metabolic assessment is an incomplete workup that leaves the patient guessing. Read more on diagnosis to understand how the right investigation changes what gets found and what gets done about it.
Why Choose Dr. Vipulroy Rathod
Dr. Vipulroy Rathod has been performing EUS-guided celiac plexus neurolysis for over 30 years at Fortis Hospital Mulund, with enough case volume to know where the procedure works well, where it doesn’t, and what the realistic expectations are for each patient rather than offering blanket reassurance, trained physicians from 35 countries in exactly this. Patients arrive on heavy opioid loads in significant pain and most leave with a picture that looks completely different within days, not because the cancer changed but because the nerve driving the pain was finally addressed directly.
Start Your Treatment Journey Today
Frequently Asked Questions
Patients with unresectable pancreatic cancer causing severe pain not controlled by oral analgesics are the primary candidates for this procedure.
Pain relief typically lasts weeks to months and can be repeated if pain returns as disease progresses over time.
Yes, generally safe when performed by an experienced endoscopist with serious complications rare though temporary diarrhoea and hypotension can occur.
Neurolysis uses alcohol for permanent nerve destruction while block uses steroids or local anaesthetic for temporary relief lasting weeks rather than months.
Reference links-
- EUS Celiac Plexus Neurolysis Guidelines — American Society for Gastrointestinal Endoscopy
- Pancreatic Cancer Pain Management — World Gastroenterology Organisation
