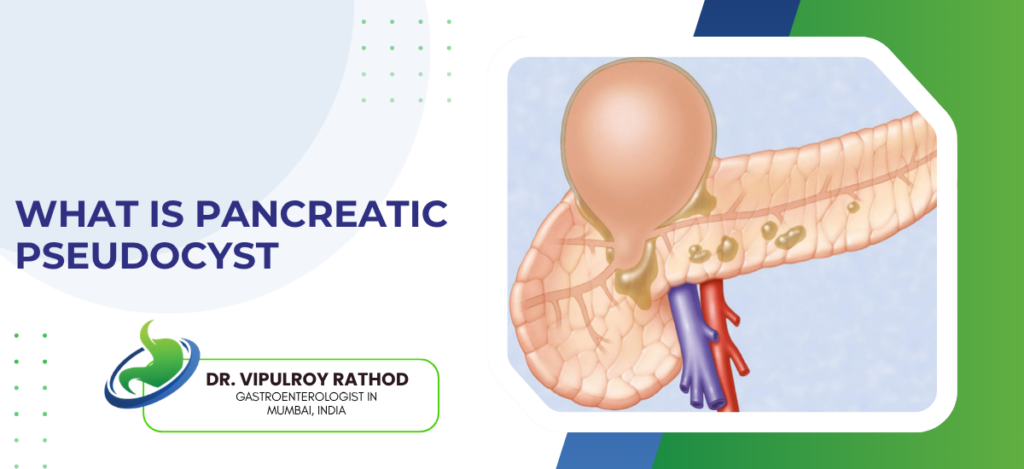
A pancreatic pseudocyst is a fluid-filled sac that forms near the pancreas after an episode of pancreatitis or pancreatic injury, and unlike a true cyst it doesn’t have an epithelial lining which is why it gets the “pseudo” tag. Most develop weeks after acute pancreatitis when leaked pancreatic juice gets walled off by surrounding tissue, and while some vanish on their own the ones that stick around or keep growing can cause real problems that need dealing with.
According to Dr. Vipulroy Rathod, an experienced Gastroenterologist in Mumbai, “Patients panic when they hear the word cyst near their pancreas but pseudocysts are not cancerous and in many cases don’t even need treatment, though the ones that do need treating are best handled endoscopically now rather than surgically which is a massive shift from how things were done even fifteen years ago.”
Why do they form and what do they feel like?
Pancreas leaks digestive juice when it gets inflamed or banged up and that fluid has to go somewhere, so the body walls it off with inflammatory tissue creating a pocket that either gets reabsorbed quietly or grows big enough to start making its presence felt.
- After acute pancreatitis: Most common setup where the gland gets inflamed, juice leaks, and over 4 to 6 weeks the body wraps inflammatory tissue around the puddle creating a walled-off collection that shows up as a dark round pocket on CT or ultrasound that wasn’t there before.
- After chronic pancreatitis: Duct blockages from scarring or stones force juice to back up and leak out through smaller ducts, and these pseudocysts have an annoying habit of coming back because the underlying duct problem hasn’t gone anywhere so new collections keep popping up even after the old ones get drained.
- After pancreatic injury: Abdominal trauma or surgical damage can bust a duct open and cause fluid to pool and collect, and while these behave similarly to post-pancreatitis ones the management sometimes takes a different turn depending on exactly where the duct got wrecked.
- Symptoms: Small ones often cause absolutely nothing and get caught by accident on imaging done for something unrelated, while bigger ones lean on surrounding structures causing upper belly pain, nausea, feeling full after two bites of food, and sometimes vomiting if the collection gets large enough to squash the stomach flat.
If symptoms have been hanging around after a pancreatitis episode, our pancreatitis treatment page covers what management looks like including what happens when complications like pseudocysts show up and won’t go away.
How do they get treated?
Not every pseudocyst needs someone going after it and jumping in too early on a collection that would’ve sorted itself out is one of the oldest mistakes in managing these, so the first call is always whether to do something or whether to sit tight and let the body handle it.
- Watch and wait: Small quiet ones under 4 to 6 cm that aren’t growing and aren’t bugging the patient often pack up and leave on their own within weeks to months, and the smart move is serial imaging to track what’s happening rather than rushing to drain something that might just vanish if everyone keeps their hands off it.
- Endoscopic drainage: When the pseudocyst is mature enough with a decent wall and is sitting close to the stomach or duodenum, an endoscopist punches a hole between the cyst and the gut using EUS guidance, drops stents through that hole, and lets the fluid drain internally which has basically taken over from surgery as the go-to approach for most cases now.
- Percutaneous drainage: External drain placed through the skin under imaging guidance when the collection can’t be reached with a scope or the patient is too crook for endoscopy, though it comes with a higher fistula risk and generally takes longer to fully wrap up compared to going in through the gut.
- Surgery: Saved for pseudocysts that can’t be accessed any other way, cases where a disconnected duct segment needs surgical plumbing repair, or situations where the collection has gotten complicated with bleeding or infection that isn’t responding to anything less invasive.
Telling pseudocysts apart from other pancreatic findings matters because the management couldn’t be more different for each, and our pancreatic cancer vs pancreatic cyst blog covers how various pancreatic lesions get evaluated and why nailing the distinction early changes everything about what happens next.
Why choose Dr. Vipulroy Rathod for pseudocyst management?
Dr. Vipulroy Rathod has over 30 years in advanced gastroenterology with more than 80,000 endoscopic procedures behind him, and EUS-guided pseudocyst drainage is one of those procedures where the gap between someone who’s done hundreds and someone who’s done a dozen shows up directly in the results because threading a stent into a fluid collection millimetres from major blood vessels under ultrasound guidance isn’t the kind of thing that goes well when the operator is still figuring it out.
What patients get here is an honest assessment of whether the pseudocyst actually needs draining or whether leaving it alone is the smarter play, because the itch to intervene on every collection that pops up on a scan is strong but experienced operators know that a good chunk of these sort themselves out and the real skill is telling which ones won’t.
Book your consultation today with one of India’s most experienced specialists for pancreatic pseudocyst evaluation.
Frequently Asked Questions
A pseudocyst is a fluid-filled pocket near the pancreas that forms after pancreatitis or pancreatic injury, walled off by inflammatory tissue rather than a proper lining which is what makes it different from a true cyst.
Plenty of small quiet ones sort themselves out within weeks to months without anyone touching them, and treatment only comes into play when they hang around, keep growing, cause symptoms, or pick up complications like infection or bleeding.
Most get drained endoscopically using EUS guidance to punch a hole between the pseudocyst and the stomach or duodenum, with stents dropped through to let fluid drain internally which skips any external cuts entirely.
They absolutely can especially when the root cause like chronic pancreatitis or a busted pancreatic duct hasn’t been sorted out, which is why fixing the underlying problem alongside draining the collection is what actually stops the cycle from repeating.
Reference links-
- Pancreatic Pseudocyst Management Guidelines — American College of Gastroenterology
- EUS-Guided Pseudocyst Drainage Evidence — National Library of Medicine
