
Most people have dealt with that uncomfortable, heavy feeling after a big meal at some point. But what happens when it’s not just once in a while — what if it happens every single time you eat, regardless of what’s on your plate? That’s when indigestion stops being a passing inconvenience and starts becoming a real problem worth investigating.
Medically, this condition is referred to as dyspepsia. It’s not a disease on its own, but rather a collection of symptoms that point toward something going wrong in the digestive process. For some people, it’s been going on for years, and they’ve simply learned to live with the discomfort — which, unfortunately, is not the right approach.
Dr. Vipulroy Rathod, a globally recognized gastroenterologist in Mumbai, India, puts it plainly:
“When patients visit me and tell they have indigestion after every meal, my first advice to them is you must not accept this as normal. Persistent dyspepsia is your gut’s way of communicating that something is not functioning properly. Most of the time, after we figure out the root cause, treatment is quite easy. However, if it remains untreated for a long time, the situation can become more and more complicated.”
Dr. Rathod has been a source of help to patients from India and around the world who suffer from chronic digestive problems by helping them get rid of these problems permanently. His method is not only about relieving symptoms rather, it is about finding out the reason behind them.
What Exactly Is Indigestion and Why Does It Keep Happening?
The stomach matters a lot in digestion. When you eat, it starts working right away, producing acid, contracting muscles to break down food. These processes happen without you thinking about them. But sometimes, the stomach can’t handle what you’re eating. You feel a burning in your chest or notice food just sitting there without moving through. If this happens after every meal, something’s wrong. It’s not a one-off issue There’s a pattern. Something consistently messes with digestion. The problem isn’t temporary. You need to figure out what’s causing it – before symptoms get worse.
What Could Be Causing It? Common Reasons Behind Post-Meal Indigestion
There’s rarely one single explanation. Several conditions — some quite common, others less so — can lead to indigestion that shows up meal after meal:
Acid Reflux or GERD
Gastritis
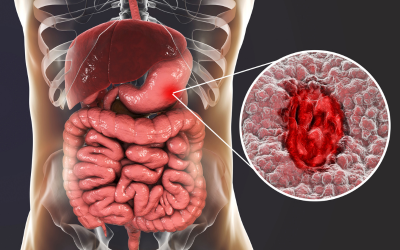
Peptic Ulcers
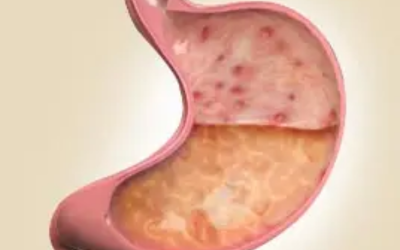
Functional Dyspepsia
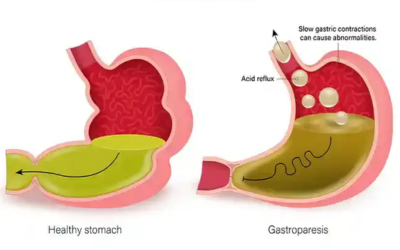
Gastroparesis
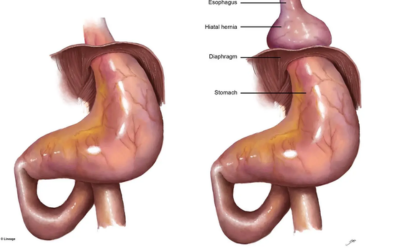
Hiatal Hernia

Food Intolerances
Eating Habits
Understanding which of these applies to you is what drives the treatment decision.
Symptoms That Tell You It's More Than Just Overeating
There’s a difference between feeling a bit full after a heavy meal and experiencing symptoms that follow you after every sitting, no matter what or how much you’ve eaten. Here’s what to pay attention to:
- Burning or aching in the upper abdomen — not just heartburn, but a deeper discomfort that starts during or shortly after eating.
- Bloating that doesn’t go away quickly — a sense of tightness or pressure in the stomach that can last for hours.
- Nausea — sometimes mild, sometimes strong enough to put you off food entirely.
- Frequent belching or gas — the body’s attempt to release built-up pressure in the stomach.
- Feeling full after just a few bites — known as early satiety, this is particularly associated with gastroparesis and functional dyspepsia.
- Regurgitation — food or acid coming back up, sometimes with a sour or bitter taste.
- Heartburn — a burning feeling that travels from the stomach up into the chest or throat.
Dr. Rathod advises that if any of these symptoms are accompanied by significant weight loss, difficulty swallowing, blood in the stool, or persistent vomiting, medical evaluation should not be delayed. These could point to something more serious that requires urgent attention.
Treatment: What Actually Helps With Chronic Indigestion?
The good news is that most causes of chronic indigestion are very treatable. The approach depends on what’s been found:
- Acid-reducing medications such as proton pump inhibitors (PPIs) or H2 blockers are commonly prescribed for GERD, gastritis, and ulcer-related indigestion.
- Antibiotics combined with acid suppressants are used specifically to clear pylori infections.
- Prokinetics — medications that help the stomach contract and empty more efficiently — are useful when gastroparesis or slow digestion is the issue.
- Dietary adjustments are almost always part of the plan. Reducing fatty foods, spicy dishes, caffeine, and carbonated drinks removes a lot of the strain on an already irritated gut.
- Stress management plays a bigger role than most people expect. The gut and brain are deeply connected, and chronic stress is a genuine driver of functional digestive issues.
- Endoscopic treatment may be required in some cases — for instance, when a hiatal hernia needs correction or when ulcers require intervention.
Dr. Rathod works with each patient to build a plan that’s practical and sustainable, not just a short-term fix.
Simple Changes That Can Make a Significant Difference
Alongside medical treatment, daily habits have a real impact on how well the digestive system functions:
- Slow down at mealtimes. Eating quickly means swallowing more air and giving your stomach less time to signal fullness. It’s a small change with a noticeable effect.
- Don’t lie down right after eating. Give your body at least two to three hours upright after a meal before resting.
- Watch your portions. Smaller, more frequent meals tend to be gentler on the digestive system than large, infrequent ones.
- Cut back on common triggers. Fried food, alcohol, caffeine, and carbonated drinks are worth reducing — at least while symptoms are being managed.
- Stay active. Even light walking after meals helps with gastric motility and reduces bloating.
- Don’t overuse antacids without guidance. Regular, unsupervised antacid use can mask symptoms and, in some cases, cause longer-term damage to the stomach lining.
Frequently Asked Questions
Reference Links:
- https://www.niddk.nih.gov/health-information/digestive-diseases/indigestion-dyspepsia
- https://my.clevelandclinic.org/health/diseases/7522-indigestion
Disclaimer: The information shared in this content is for educational purposes and not for promotional use.
