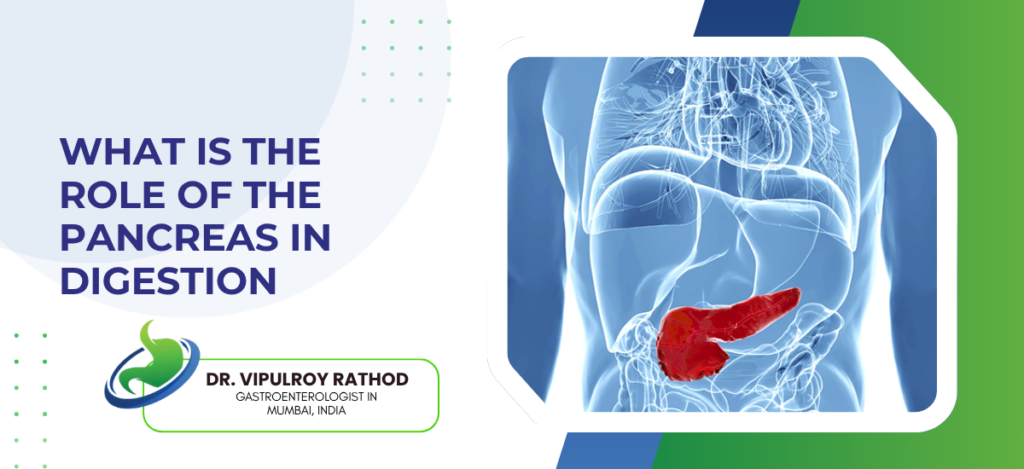
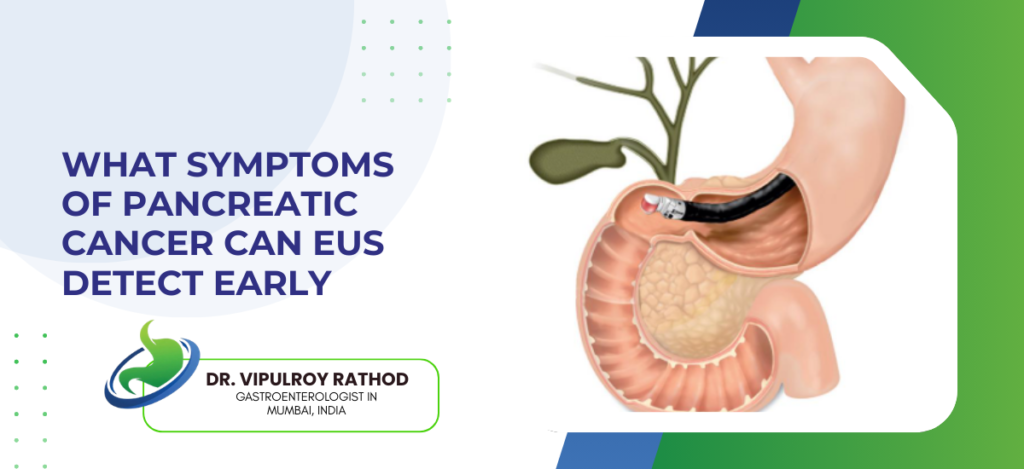
Does Smoking and Alcohol Increase Digestive Cancer Risk
Yes, smoking and alcohol significantly increase the risk of developing digestive cancers, acting independently and combining to magnify the danger. Tobacco is directly linked to oesophageal, stomach, pancreatic, and colorectal cancer while alcohol causes chronic inflammation and tissue damage, raising risk for liver, oesophageal, stomach, and colorectal cancers. According to Dr. Vipulroy Rathod, an experienced Gastroenterologist in Mumbai, “Smoking and alcohol are not just general health risks, they are direct carcinogens for the digestive tract and patients who combine both habits are in a risk category that warrants active surveillance, not just lifestyle advice.” How Does Smoking Increase Digestive Cancer Risk? Tobacco carcinogens don’t stay in the lungs. They travel through the bloodstream, hit the liver, and make contact with digestive tract lining at multiple points along the way. Oesophageal Cancer, Direct Contact: Tobacco smoke and chewing tobacco expose oesophageal lining directly to nitrosamines and risk of squamous cell carcinoma in smokers runs roughly 3 to 5 times higher than non-smokers, climbing further with duration and quantity. Stomach Cancer Gets Worse with H. Pylori: Smoking independently raises stomach cancer risk but also makes existing H. pylori infection more aggressive and harder to eradicate, so a smoker with H. pylori is in a meaningfully worse position than a non-smoker with the same infection. Pancreatic Cancer, Risk Doubles: One of the most consistent findings across studies is that smoking roughly doubles lifetime pancreatic cancer risk and it doesn’t drop back to baseline quickly on quitting, around 10 years of cessation before risk normalises significantly. Colorectal Cancer Builds Over Decades: Risk becomes statistically significant after 30 to 40 pack-years, which means patients who smoked heavily in their 20s and 30s are in a higher colonoscopy surveillance category now even if they stopped years ago. Habit history matters as much as current habits. Specialist in GI cancer treatment factors in cumulative exposure not just what you’re doing today. How Does Diabetes Increase Pancreatic Disease Risk? Alcohol is a Group 1 carcinogen. No safe level for cancer risk has been established and the GI tract takes the most direct hit of any organ system. Liver Cancer Through Cirrhosis: Chronic alcohol use causes cirrhosis and cirrhosis is the strongest single risk factor for hepatocellular carcinoma, cirrhotic patients carry a 1 to 5% annual liver cancer risk regardless of whether they’ve stopped drinking by that point. Colorectal Cancer, Even Moderate Drinking: Risk rises linearly with consumption and even 1 to 2 drinks per day is associated with measurably increased colorectal cancer risk in large population studies, something most patients are genuinely surprised to hear when told directly. Oesophageal Cancer with Smoking Combined: Alcohol and tobacco act synergistically on oesophageal tissue and the combined risk is multiplicative not additive, heavy drinkers who smoke sit in a risk category that justifies regular upper endoscopy surveillance rather than waiting for symptoms to show up. Stomach Cancer Through Mucosal Damage: Alcohol directly damages gastric mucosal lining and chronic exposure creates persistent inflammation that increases H. pylori susceptibility and accelerates the gastritis to cancer progression sequence faster than either factor alone. Both together are worse than either alone and risk doesn’t reset quickly after stopping. Read more on AI in GI endoscopy to understand how modern detection tools are changing early cancer surveillance. Why Choose Dr. Vipulroy Rathod Dr. Vipulroy Rathod has 30 years in gastroenterology and EUS since 1998. Trained physicians from 35 countries. Sees smoking and alcohol-related GI cancers regularly at Fortis Hospital Mulund and investigates them properly rather than managing symptoms while the underlying malignancy goes undetected.Patients with decades of combined habits and vague GI symptoms come in regularly. Most leave with a clear picture of what’s actually happening. Better than finding out later when options narrow. Start Your Treatment Journey Today Book Appointment Call now Frequently Asked Questions Which digestive cancer is most strongly linked to smoking? Oesophageal, pancreatic, and stomach cancers have the strongest established links to smoking among digestive cancers. Does quitting smoking reduce digestive cancer risk? Yes, risk decreases progressively after quitting though for pancreatic cancer it takes around 10 years to approach baseline. Is any amount of alcohol safe from a digestive cancer perspective? No safe threshold has been established. Even moderate alcohol consumption is associated with increased colorectal and liver cancer risk. How soon after stopping alcohol does liver cancer risk reduce? Risk reduces gradually but cirrhosis-related liver cancer risk persists even after alcohol cessation in already-cirrhotic patients. Reference links- Alcohol, Tobacco and GI Cancer Risk — World Gastroenterology Organisation Smoking and Digestive Cancer Evidence — American College of Gastroenterology
Does Smoking and Alcohol Increase Digestive Cancer Risk Read More »